CARDIOLOGY
Heart Failure
Clinical Guidelines and Resources
Sign up for Figure 1 and be notified directly of new clinical cases and related research, CME activities, quizzes, news, and trends. It’s free!

Figure 1, 2, 3

1. Sodium-glucose cotransporter-2 inhibitors are currently included in the medical therapy for heart failure with reduced ejection fraction

2. Several prior recommendations for hypertension, atrial fibrillation, ARB usage, and avoidance of nitrates or phosphodiesterase-5 inhibitors have been renewed

3. New guidelines for amyloid heart disease include monoclonal light chains screening, bone scintigraphy, genetic sequencing, tetramer stabilizer therapy, and anticoagulation
Summary
The American College of Cardiology (ACC) and the American Heart Association (AHA) released the updated clinical guidelines in 2022 on the management of heart failure, replacing the 2017 update. The following is a brief overview of the most relevant recommendations for cardiologists and other healthcare professionals.
Heart failure, or HF, is still the major cause of morbidity and mortality worldwide. The updated heart failure guidelines present treatment recommendations for these patients based on the most recent evidence. The recommendations provide an evidence-based strategy for managing heart failure patients, with the goal of improving quality of care and aligning with patients’ interests.
Heart Failure Clinical Guidelines and Resources
The guideline contains different areas of focus, including: prevention of HF; management strategies of HF patients in stage C, containing new treatments such as sodio-glucose cotransporte-2 inhibitors (SGLT2i) and angiotensin receptor-neprilysin inhibitors (ARNi); atrial fibrillation (AF) ablation; management of HF and secondary mitral regurgitation, including transcatheter edge-to-edge repair; specific strategies for cardiac amyloidosis and cardio-oncology management; implantable devices; and applications of left ventricular assist device (LVAD) in stage D HF patients.
The guidelines for management of heart failure describe the ACC/AHA stages of HF, the New York Heart Association (NYHA) parameters, the classification of HF by left ventricular ejection fraction (LVEF), and diagnostic algorithms for HF classification, including relevant analysis such as natriuretic peptides and cardiopulmonary exercise testing (CPET). Furthermore, updated epidemiology and causes of HF, including trends in mortality and hospitalization, and racial and ethnic disparities, are described.
Clinical assessment with the history and physical examination of the HF patients are fully described with reference studies and levels of recommendation. Important procedures for initial laboratory testing, including B-type natriuretic peptide (BNP) and N-terminal prohormone of BNP (NT-proBNP) highlight the importance of biomarkers for prevention, initial diagnosis, and risk stratification of patients. Electrocardiographic (ECG) with a 12-lead ECG is also indicated as a fundamental part of the initial encounter to optimize the management.
Novel molecular testing, including genetic evaluation and screening, is also recommended for some conditions such as inherited cardiomyopathies, aiming to decrease HF progression and sudden death. Conversely, invasive evaluation such as endomyocardial biopsy was recommended only for some specific cases.
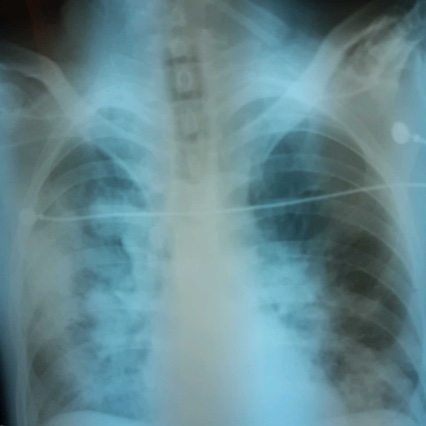
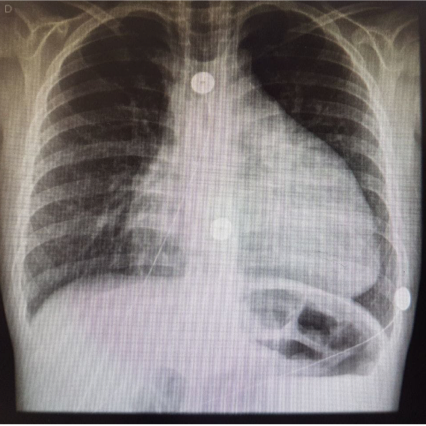
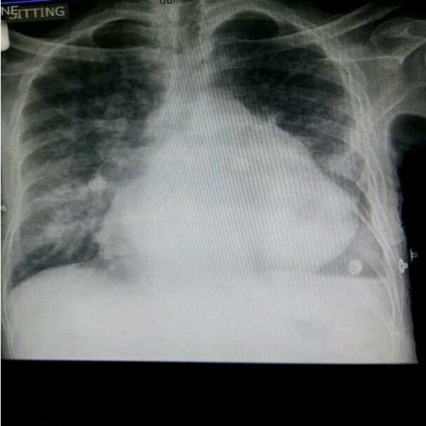
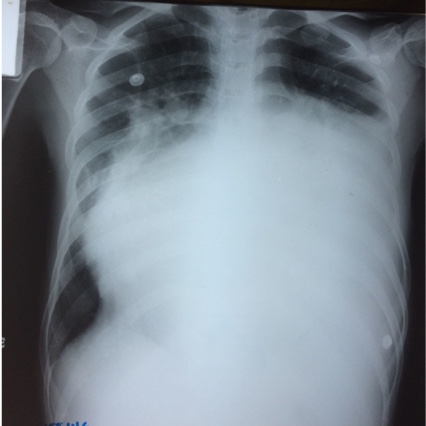
Cardiac imaging plays an important role in the recommendations presented in the 2022 guidelines. A chest X-ray is recommended to determine the size of the heart and the presence of pulmonary congestion. Furthermore, the recommendations for transthoracic echocardiography (TTE) for the initial assessment of cardiac structure and function were described by the committee. Additional cardiac imaging technologies, including cardiac magnetic resonance (CMR) and cardiac computed tomography (CT) for LVED, are also recommended in some cases for management of heart failure.
After extensive recommendations on the diagnostics, classification, risk stratification, and monitoring procedures of HF patients, the guidelines summarize the most appropriate treatment strategy for each group of patients. The recommendation for stage A of HF includes the management of comorbidities such as hypertension and diabetes with SGLT2i, lifestyle modification, and other strategies. For stage B, additional recommendations were highlighted, such as beta-blockers, angiotensin-converting enzyme inhibitors or angiotensin receptor blockers, and implantable cardioverter-defibrillators for some patients. Relevant potential barriers to effective self-care were also described, such as depression, frailty, and low social support, among other factors that might influence the management of heart failure.

Full Guidelines
Read the most recent full guidelines for clinical management of heart failure: American College of Cardiology clinical guidelines on the management of heart failure.

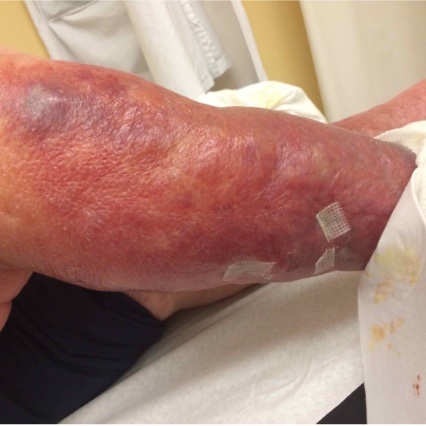
Heart Failure Patient Cases
Click on the image to see the full case details and sign in to view community comments.
See more cases like these
Sign up for Figure 1 and gain access to a library of 100,000+ real-world cases.

Heart Failure Clinical Quiz
Take this quiz in the app to test your knowledge and view community comments.
ww Quick Quizw
How well do you understand hypothermia protocol for cardiac events?
A 32-year-old with a history of a recent non-surgical metatarsal fracture presents to the emergency department after pulseless electrical activity cardiac arrest.The patient was intubated in the field and coded on the way to the hospital for 10 minutes prior to the return of spontaneous circulation (ROSC). Upon arrival to the emergency department, the patient is started on vasopressors. Pulmonary angiography confirmed the suspected diagnosis of a pulmonary saddle embolus and the patient is prepped for a thrombectomy. Following the procedure and prior to transfer to intensive care unit, the patient is started on a hypothermia protocol — also known as therapeutic hypothermia.

Learn by Listening
Code Blue DDx Podcast Episode
Hear about the journey of an 8-year-old diagnosed with a rare inherited disease that drastically affects his heart.


Related Research
2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines | PubMed
“The 2022 guideline is intended to provide patient-centric recommendations for clinicians to prevent, diagnose, and manage patients with heart failure … A comprehensive literature search was conducted from May 2020 to December 2020, encompassing studies, reviews, and other evidence conducted on human subjects that were published in English from MEDLINE (PubMed), EMBASE, the Cochrane Collaboration, the Agency for Healthcare Research and Quality, and other relevant databases.”
A Year in Heart Failure: An Update of Recent Findings | PubMed
“Major changes have occurred in these last years in heart failure (HF) management. Landmark trials and the 2021 European Society of Cardiology guidelines for the diagnosis and treatment of HF have established four classes of drugs for treatment of HF with reduced ejection fraction … These drugs consistently showed benefits on mortality, HF hospitalizations, and quality of life.”
Biomarkers for the Diagnosis and Management of Heart Failure | PubMed
“Heart failure (HF) is a significant cause of morbidity and mortality worldwide. Circulating biomarkers reflecting pathophysiological pathways involved in HF development and progression may assist clinicians in early diagnosis and management of HF patient … Multi-marker scores and genomic, transcriptomic, proteomic, and metabolomic analyses could further refine HF management.”

Related Medical Calculators

Gustavo Monnerat, PhD
Scientist, Federal University of Rio de Janeiro and National Institute of Cardiology