
Between the late nights and the challenging nature of medicine, the life of a healthcare professional can be an exhausting one. And as the pandemic wears on, the sense of burnout only worsens.
To better understand the experiences of healthcare professionals, we conducted a burnout in healthcare survey asking the community for insights on contributing factors, symptoms, support, and the overall impact. With this data, the industry can better identify burnout and also start to address it.
Here’s what more than 100 healthcare professionals had to say.
The Severity of Burnout in Healthcare
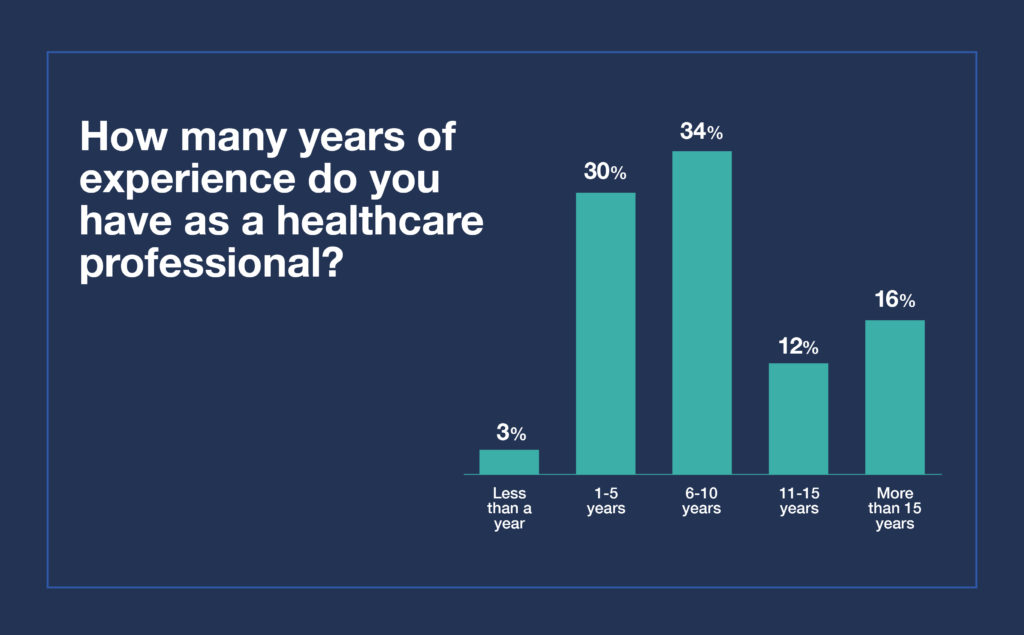
Of the respondents, 16% have more than 15 years of experience, 34% have six to 10 years of experience, 30% have one to five years of experience, and 3% have less than a year of experience.
Almost half (43%) of respondents ranked their experience with burnout in healthcare over the past year as a four out of five (five being most severe). Those with more than 15 years of experience seem to be impacted most severely, with 40% of respondents ranking their level of burnout as a five. Of all respondents, only 3% said they have not experienced burnout in the past year.

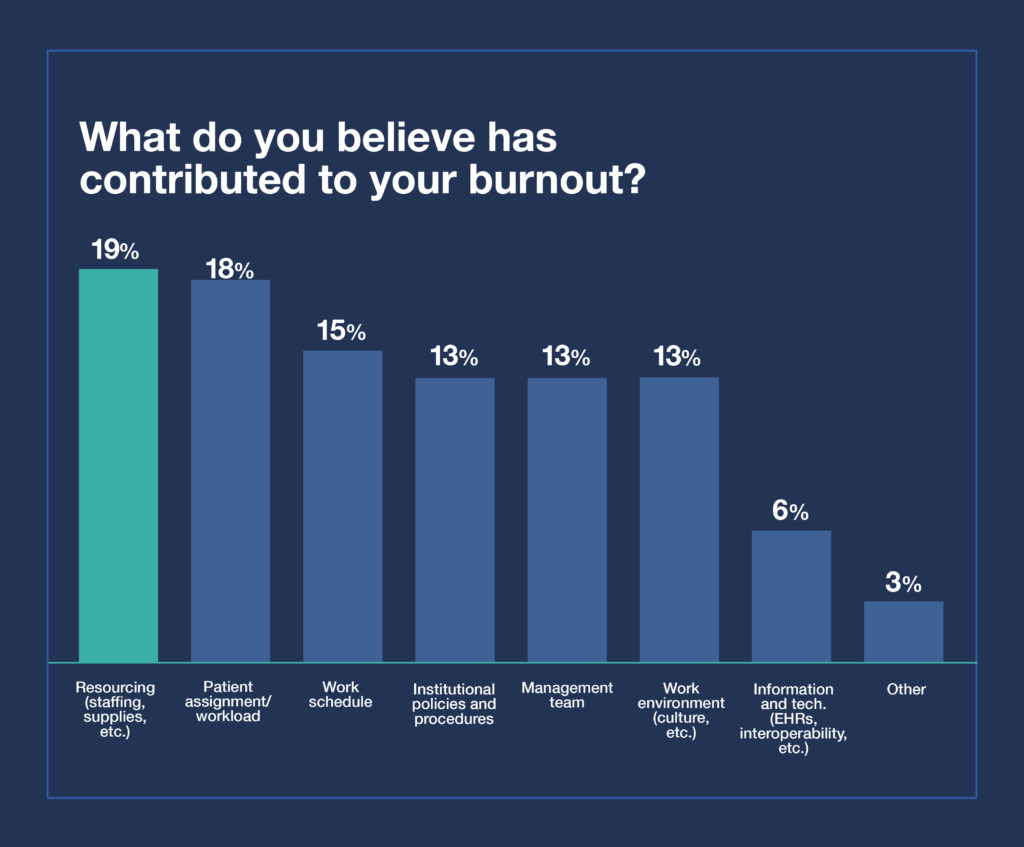
Contributing Factors of Burnout in Healthcare
When asked what has contributed to their burnout, two factors stood out: resourcing (19%), and patient assignment and workload (18%).
The Impact of Burnout
The impact of burnout is heavy. Common symptoms included depression, anxiety, lack of motivation, and fatigue.

“Depression, hopelessness, struggling to provide good patient care. Always worrying I forgot something important but not having the drive to make sure I didn’t. Feeling very passive like learned helplessness. Worry about losing my home.”
“From headaches, to stomach pain, to freezing in terror. It’s the first time in 20 years that I have reconsidered my career choice.”
“I have had feelings of dread and anxiety on the nights I work. The expectation of nurses taking on more responsibility with less help makes an unsafe environment for the very people we are supposed to care for and keep safe. The stress of this has led to physical and mental exhaustion.”
Available Support and the Barriers to Use
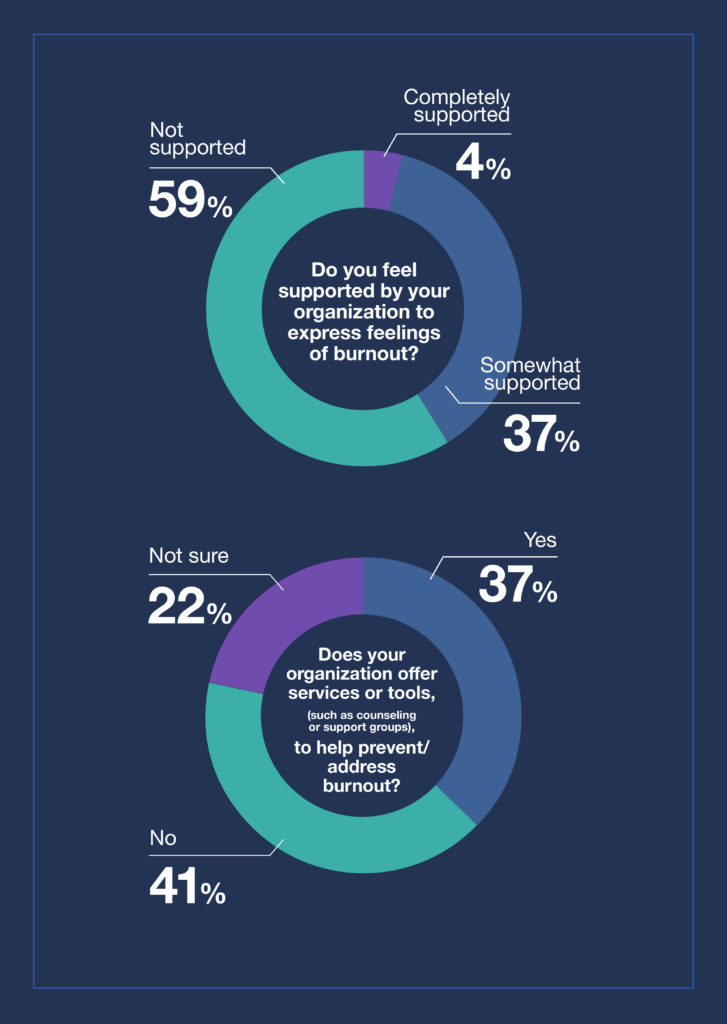
Unfortunately, when asked if they feel supported by their organization to express feelings of burnout, 59% of respondents said no, with only 4% saying they feel completely supported.
As for support services or tools offered by their organization, 37% of respondents said their organization does provide support options.
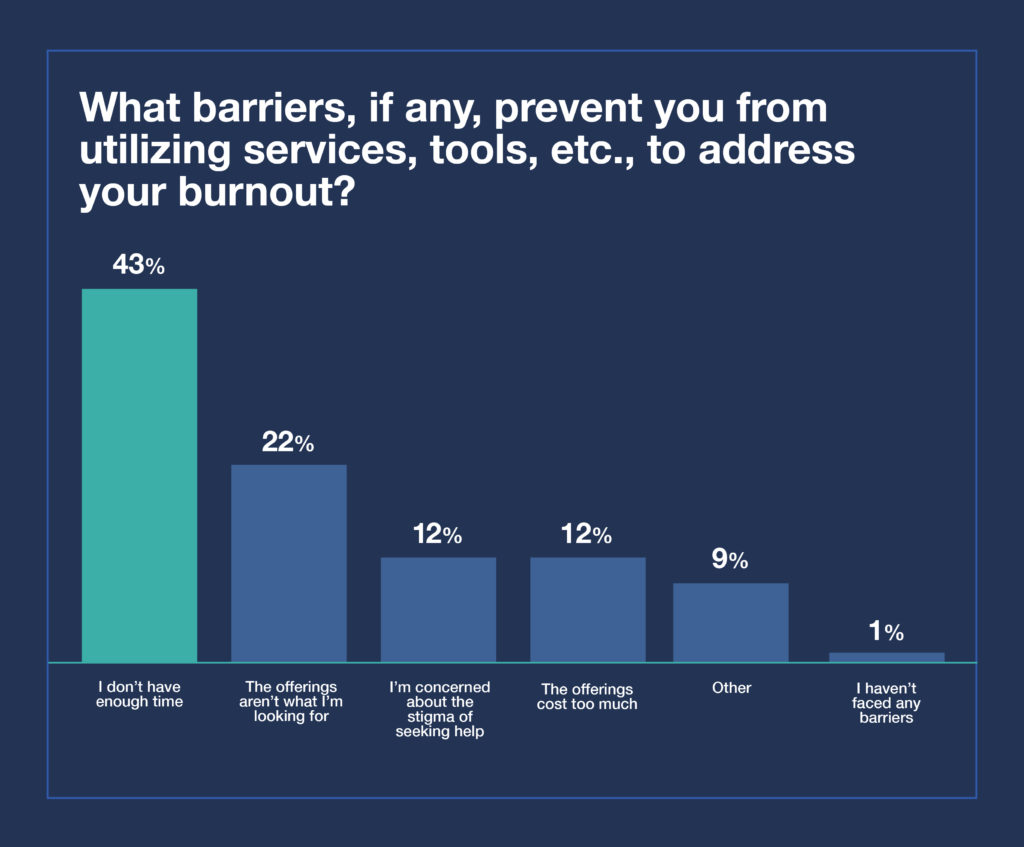
We also asked about barriers to utilizing support. Not surprisingly, almost half (43%) said their primary barrier is not having enough time.
Managing Burnout
Despite a lack of support, healthcare professionals are finding ways to manage their burnout. Many respondents noted the importance of seeking counseling, setting boundaries, and leaning on their support system.

“Workflow adjustments, counseling and support groups, actually breaking the ice and starting the conversation on this topic.”
“I personally like to compliment one staff member per day (due to us all being overwhelmed), and setting healthier limits and boundaries as necessary.”
“Doing things that previously brought joy, sitting at the beach in silence, reading books, laughing with family, talking about the stress with someone.”
The Impact of Burnout on the Workforce and Working Toward Solutions
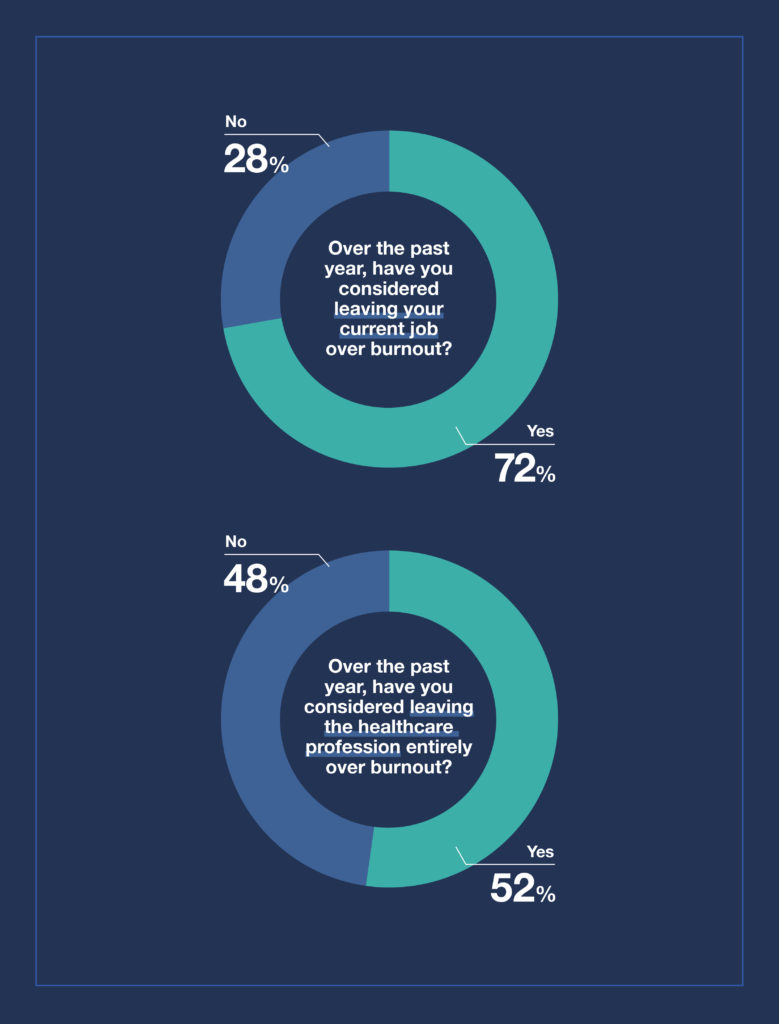
When asked if their experience with burnout in healthcare has led them to consider leaving their current job, the results were not shocking. The majority (72%) considered leaving their job over the past year.
But the responses to leaving the profession entirely were split. Of respondents, 52% said they have considered leaving the profession, while 48% said they have not.
For an industry already forecasting a workforce shortage, the impact of burnout could become dire.
In a blog post from our guest writer, Chelsie Smith, BSc, MA, and a PhD candidate, Smith shared ways organizations can help their staff through this challenging time, but also in the long term.
- Reduce the need to search for the materials necessary to do one’s job
- Reduce patient load and clustering similar cases
- Allow employees greater control over what shifts they take
- Provide, if at all possible, resources to help individuals in their home lives
- Provide a range of ways that employees can speak up about the challenges they are facing
Published February 24, 2022
Join the Conversation
Register for Figure 1 and be part of a global community of healthcare professionals gaining medical knowledge, securely sharing real patient cases, and improving outcomes.


