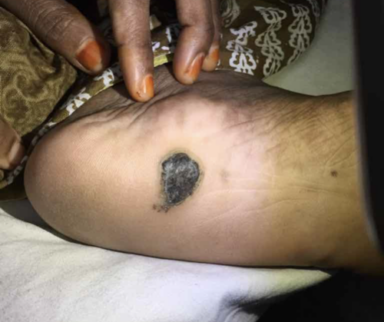
What is Hidradenitis Suppurativa?
Hidradenitis suppurativa, or HS – also known as acne inversa or Verneuil’s disease – is a chronic inflammatory condition of the skin that appears as recurrent lesions in the intertriginous areas of the body. These intertriginous areas are anatomic regions where adjacent skin surfaces make contact with each other and include the axillae, anogenital and perineal regions, and the inframammary folds, amongst others. These areas are subject to high degrees of mechanical stress and can lead to inflammation of the folliculopilosebaceous unit (FPSU).
The FPSU consists of three units: the follicular unit, which is the most superficial region at the skin surface; the pilar unit, which contains the hair follicle and papillae; and the sebaceous unit, which contains the sebaceous glands and sebum producing cells. In patients susceptible to HS, these units undergo a cytokine-mediated hyperinflammation process causing hyperkeratosis and resulting follicular unit blockage. Further inflammation and cyst formation occurs that can result in sinus tract formation between neighboring FPSUs. Over time, this can result in severe scarring and contracture.
Epidemiology
While HS is a rare condition affecting up to 4% of the population and generally thought to have a contributory genetic component, cases have been on the rise in the last decade. Non-modifiable risk factors include postpubertal and premenopausal women, with a 4:1 female-to-male ratio. There is also an increased incidence in the Black population. Modifiable risk factors include both obesity and smoking, due to increased propensity for mechanical friction and a heightening of systemic inflammation, respectively.
HS also is associated with a wide degree of medical conditions, especially those with an inflammatory component. Crohn disease is one of the most commonly associated conditions and patients with HS may be recommended to have screening for the disease. Some common comorbidities include: diabetes mellitus and metabolic syndrome, arthritis, spondyloarthropathy, polycystic ovarian syndrome (PCOS), trisomy 21 (Down syndrome), and various cancers. Patients should be screened for squamous cell carcinoma due to the possible similar appearance of the lesions. Importantly, because hidradenitis suppurativa can cause severe cases of pain and distortions of one’s appearance, all patients must be screened for depression.
Clinical Features
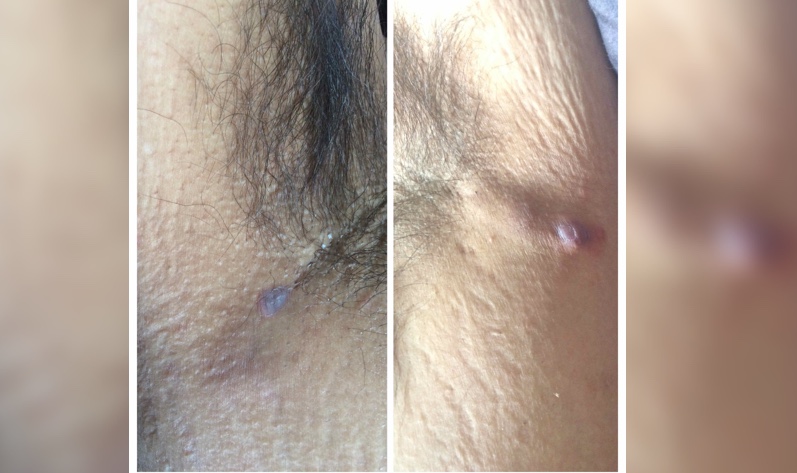
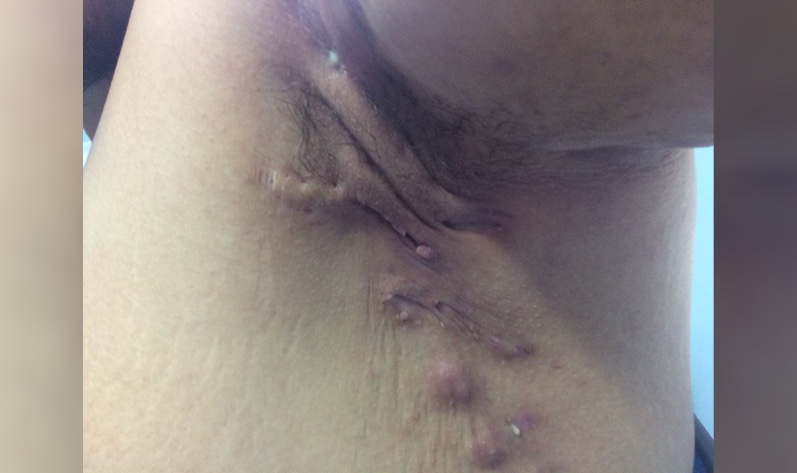
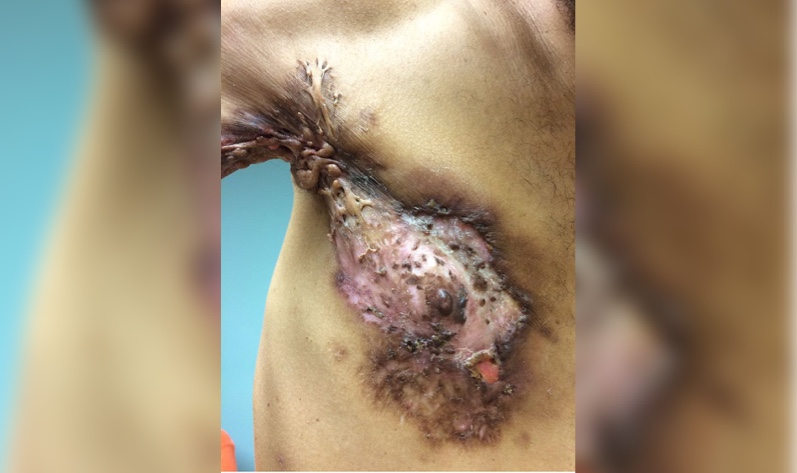
Clinical features of hidradenitis suppurativa can be diverse, especially in new onset or mild cases. The lesions range from comedones and small inflammatory nodules to scattered abscesses and tombstone comedones with interconnected sinus tracts. The more severe cases present with recurrent diffusely connected abscesses resulting in scarring and significant contracture of the dermis. As noted earlier, the lesions occur in the intertriginous regions, with the axillae being most common. Other locations include areas susceptible to increased friction from clothing, such as the posterior aspect of the neck and waist. Diagnosis of HS is often made if the lesions appear recurrently, with some guidelines citing two or more instances within a six-month period.
The lesions are typically associated with localized pain, erythema, or nonpurulent drainage. While discharge is most often malodorous but noninfectious, it is possible for secondary bacterial infections to occur, especially if the lesions are chronic. Staphylococcus aureus superinfection is rare but is reported.
Differential diagnosis of HS includes:
- Cutaneous Crohn disease
- Carbuncle or furuncle
- Epidermoid, dermoid, and pilonidal cysts
- Lymphogranuloma venerum
- Granuloma inguinale
- Primary bacterial abscess
Staging
Staging of hidradenitis suppurativa can help to determine severity of the disease and guide treatment. The Hurley classification system is a commonly employed:
- Stage I (mild): Isolated or localized abscesses; no sinus tracks or scarring
- Stage II (moderate): Recurrent abscesses with sinus tracks and scarring
- Stage III (severe): Widespread abscesses diffusely present across bodily region with interconnected tracts and scarring
Nonmedical Management
Lifestyle modification can often alleviate the degree of severity and prolong the time to lesion recurrence. Typical interventions include smoking cessation, weight loss, management of diabetes mellitus, and adoption of loose cotton clothing. Topical treatments consist of warm compresses, topical antiseptics, antibacterial soaps, and benzoyl peroxide or chlorhexidine washes. Weight loss has been demonstrated to significantly decrease severity and should be a focus for all patients with an elevated body mass index.
Medical Treatments
Pharmacologic intervention is used in mild, moderate, and severe disease cases. Medical management can be broken down by Hurley stage.
- Hurley Stage I:
- First line: Topical clindamycin
- Second line: Add topical resorcinol; intralesional corticosteroid injection
- Hurley Stage II:
- First line: Add tetracycline to stage I regimen
- Second line: Tumor necrosis factor inhibitors (adalimumab, etanercept)
- Third line: Oral retinoid (acitretin), oral clindamycin and rifampin
Refractory cases of Hurley stage I and II can be advanced to a further Hurley stage treatment paradigm. The above protocol is to be used for initial guidance. Stage III conditions can benefit from antihormonal and other biologic and immunomodulatory treatments if warranted. Refractory stage II and all stage III cases should be referred to a dermatologist.
Surgical Options
Surgical intervention is typically saved for more severe Hurley Stage III or refractory stage II cases and ranges in complexity based on the degree and area of tissue involvement and includes:
- Incision and drainage (not widely encouraged)
- Punch debridement
- Unroofing and deroofing debridement
- Laser therapy
- Tissue sparing excision
- Wide excision
Key Takeaways
- Hidradenitis suppurativa is a recurrent chronic inflammatory condition of the folliculopilosebaceous unit
- Increased incidence in premenopausal females, Black people, smokers, and the obese
- Always screen patients for depression
- Weight loss is instrumental in decreasing disease severity
- Initial treatment includes topical antibiotics and resorcinol
- Oral antibiotics, resorcinol, hormonal therapies, immunomodulators, and biologics are added for moderate-to-severe disease
- Surgical treatment is reserved for more severe cases
Published December 13, 2021
Join the Conversation
Register for Figure 1 and be part of a global community of healthcare professionals gaining medical knowledge, securely sharing real patient cases, and improving outcomes.