Learning Objective
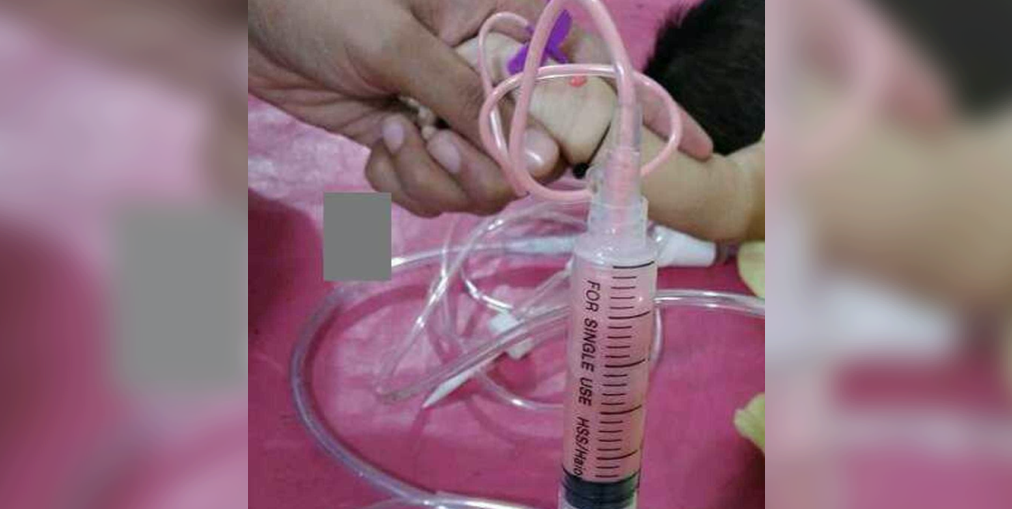
- To recognize the significance of foamy, pink blood in an infant
A 2-month-old with no notable health history presents to the emergency department with mild respiratory distress. The mother states that the child woke up in the middle of the night with a tight cough that produced a bark-like sound which seemed to improve when the infant was taken outside into the cool night air. The mother brought the child immediately to the emergency department. You evaluate the child and find mild expiratory stridor, consistent with croup. Additionally, physical exam shows mild hepatosplenomegaly.
During the blood draw the phlebotomist is alarmed because of foamy pink blood in the test tube and asks you to come see the unusually colored blood. Suspecting hyperlipidemia, you add a full lipid panel with hepatic enzymes, blood count, pancreatic enzymes, and electrolytes to the laboratory order. On further questioning, the infant’s parents were both treated for high levels of total cholesterol and triglycerides with diet and medication.
Laboratory investigation of the pink blood reveals an elevated serum cholesterol of 2,000 mg/dl (<170 mg/dl) and triglycerides of 12,200 mg/dl (<150 mg/dl). Lipase and amylase are normal, as well as hemoglobin, creatinine, and blood glucose. However, hepatic enzymes are mildly elevated at two to three times the upper limit of normal for ALT and AST with normal bilirubin. The patient was treated for croup in the emergency department with dexamethasone at 0.6 mg/kg in a single dose and admitted overnight to observe the child’s breathing. The infant was also diagnosed with familial combined hyperlipidemia and treated with fibric acid derivatives and a low triglyceride intake diet of less than 50 mg/day.
The patient recovers rapidly and is discharged the next day with a follow up scheduled two weeks later with repeat lipid studies. The child does not develop pancreatitis and repeat bloodwork shows a 50% reduction in cholesterol and triglyceride levels as well as normalization of the hepatic enzymes. The patient has no persistent sequelae of the croup diagnosis and is following appropriate developmental milestones.
Pink blood is caused by hyperlipidemia which creates a foamy-appearing, white serum giving whole blood a pink appearance. Hyperlipidemia in infants can be primary or secondary. Primary hyperlipidemia includes inherited genetic conditions such as familial combined hyperlipidemia occurring in 1-2% of the general population. Other genetic forms of hyperlipidemia include LDL receptor defects, Apo B LDL receptor defect, endothelia LPL defect, Apo C-II deficiency, lysosomal acid lipase deficiency and specific genes LCAT, ABCA 1, ABCG 5, ABCG 8 defects as well as other genetic defects. Secondary causes of hyperlipidemia that should be investigated at the time of diagnosis are diabetes, liver and kidney disease, and hypothyroidism.
Further Reading
Hypertriglyceridemia Presenting as “Pink Blood” and Elevated Hemoglobin Level
Lipemia Retinalis in a 27 Day Old Neonate: A Case Report
References
Avis HJ, Scheffer HJ, Kastelein JJ, Dallinga-Thie GM, Wijburg FA. Pink-creamy whole blood in a 3-month-old infant with a homozygous deletion in the lipoprotein lipase gene. Clin Genet. 2010 May;77(5):430-3. doi: 10.1111/j.1399-0004.2009.01369.x. Epub 2010 Jan 4. PMID: 20095985.
Chaurasiya OS, Kumar L, Sethi RS. An infant with milky blood : an unusual but treatable case of familial hyperlipidemia. Indian J Clin Biochem. 2013 Apr;28(2):206-9. doi: 10.1007/s12291-012-0285-9. Epub 2012 Dec 11. PMID: 24426212; PMCID: PMC3613496.
Originally published June 16, 2021; updated October 12, 2021
Want more clinical cases?
Join Figure 1 for free and start securely collaborating with other verified healthcare professionals on more than 100,000 real-world medical cases just like this one.