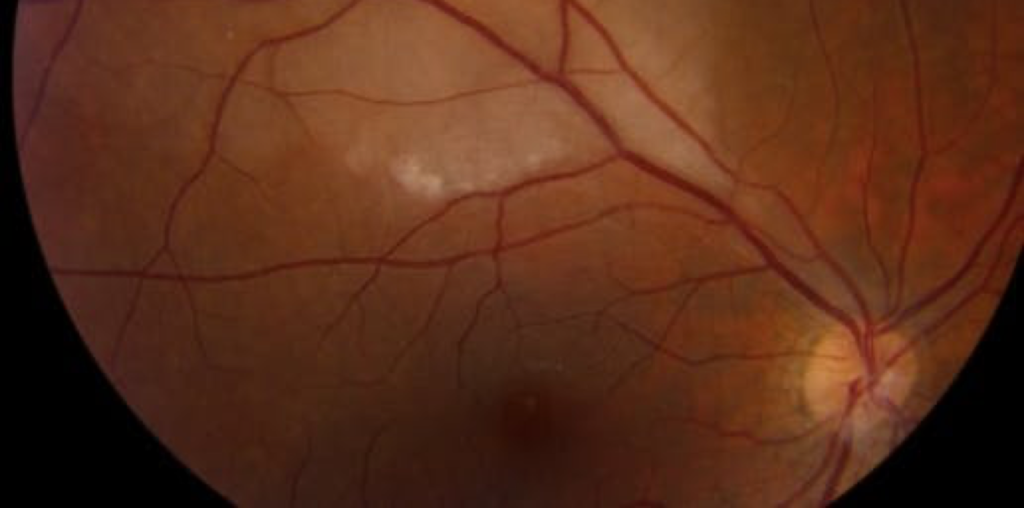
An 87-year-old with a history of polymyalgia rheumatica presents to urgent care with sudden, painless, unilateral vision loss preceded by a week of mild right-sided headache. The patient endorses difficulty chewing meat due to jaw fatigue. On exam, they have tenderness over the right forehead, normal vision in the left eye, and finger counting only in the right eye. Vision is restricted in the inferior quadrants of the right eye. The erythrocyte sedimentation rate (ESR) is 70.
Sudden vision loss in a patient over age 60 is concerning for giant cell arteritis (GCA), particularly in the context of temporal headache and jaw claudication. This patient has a branch retinal artery occlusion (BRAO), causing vision loss. Disk pallor in the distribution of a major retinal artery, as pictured, indicates ischemic damage.
High dose steroid treatment should be started empirically due to the high risk for progressive vision loss. The benefit of clot busting drugs like alteplase is uncertain at this time, although hyperacutely presenting cases should still be evaluated urgently in concert with local stroke teams. Other factors consistent with giant cell arteritis include thrombocytosis and the “halo sign” on duplex ultrasonography. Temporal artery biopsy is confirmatory.
Further Reading
Giant Cell Arteritis (Temporal Arteritis)
Ophthalmic Manifestations of Giant Cell Arteritis
References
Retinal artery occlusion – patients – The American Society of Retina Specialists [Internet]. [cited 2022 Feb 2]. Available from: https://www.asrs.org/patients/retinal-diseases/32/retinal-artery-occlusion

Kaci McCleary, MD
Hospice and Palliative Care Fellow, OhioHealth
Published February 2, 2022
Want more clinical cases?
Join Figure 1 for free and start securely collaborating with other verified healthcare professionals on more than 100,000 real-world medical cases just like this one.