Learning Objectives
- To gain knowledge of presentation and treatment of chronic scalp plaque psoriasis in adults
- To implement currently recommended treatment of chronic scalp plaque psoriasis in a clinical case scenario
A 58-year-old presents to the office with a large, raised, flaky, lesion on the scalp that has been present for three weeks. The patient also reports stiffness and pain in the left second finger for the last two weeks with difficulty removing their rings because of the swelling. Past medical history is significant for a 28-year history of relapsing-remitting plaque psoriasis with scalp lesions. The patient notes previous use of phototherapy many years ago but has only used topical therapies since. Currently, they are on no other medications.
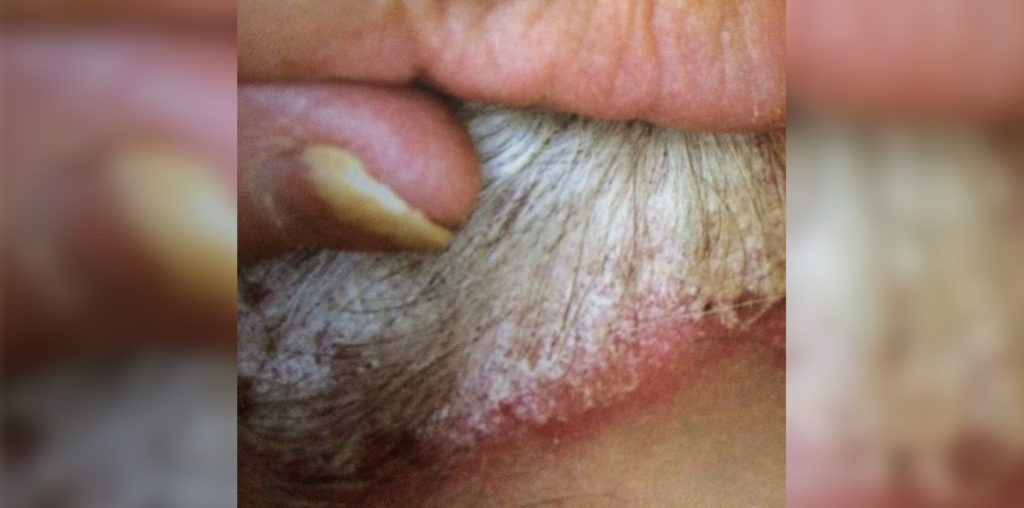
On physical exam the patient has a large, raised, well-demarcated, red and silvery appearing, flaking plaque on the occipital scalp just above the hairline. Additionally, the left second finger is visibly swollen, “sausage-shaped,” with limited movement at the proximal inter-phalangeal joint.
The patient is diagnosed with chronic scalp plaque psoriasis and concomitant psoriatic arthritis. Screening for additional psoriatic comorbidities is negative. Because of systemic symptoms, the patient is offered systemic treatment. Baseline labs reveal normal complete blood count, renal function, and hepatic enzymes. The patient has a negative PPD test for tuberculosis and negative serologies for hepatitis B and C. They are started on methotrexate 10 mg weekly and given a high potency topical steroid lotion to apply to the affected scalp daily for two weeks. After four weeks the patient notices a thinning of the scalp lesion with less flaking and irritation, and finger swelling is improved. Labs remain normal, and the patients continues on methotrexate at the same dose for an additional eight weeks, then tapers off to avoid rebound disease.
Corticosteroid foam and spray resulted in improved redness, decreased pruritus and burning compared to corticosteroid lotions, and were well tolerated from a cosmetic standpoint. With scalp lesions that are chronic and require long-term control, there is an attempt to minimize corticosteroid exposure by utilizing other methods such as vitamin D analogs, keratolytics, coal tar, and phototherapy. Several classes of systemic agents have been shown to be effective, such as methotrexate, cyclosporine, acitretin, biologics, and phosphodiesterase-4 inhibitors (PDE-4 inhibitors). Of these, methotrexate is often the most economical, although the risk of toxicity is significant and must be managed by an experienced provider.
Further Reading
References
Elmets CA, Leonardi CL, Davis DMR, Gelfand JM, Lichten J, Mehta NN, et al. Joint AAD-NPF guidelines of care for the management and treatment of psoriasis with awareness and attention to comorbidities. Journal of the American Academy of Dermatology. 2019;80(4):1073-113. doi: 10.1016/j.jaad.2018.11.058.
Menter A, Gelfand JM, Connor C, Armstrong AW, Cordoro KM, Davis DMR, et al. Joint American Academy of Dermatology-National Psoriasis Foundation guidelines of care for the management of psoriasis with systemic nonbiologic therapies. J Am Acad Dermatol. 2020;82(6):1445-86. Epub 2020/03/03. doi: 10.1016/j.jaad.2020.02.044. PubMed PMID: 32119894.
Mosca M, Hong J, Hadeler E, Brownstone N, Bhutani T, Liao W. Scalp Psoriasis: A Literature Review of Effective Therapies and Updated Recommendations for Practical Management. Dermatology and therapy. 2021;11(3):769-97.
Want more clinical cases?
Join Figure 1 for free and start securely collaborating with other verified healthcare professionals on more than 100,000 real-world medical cases just like this one.