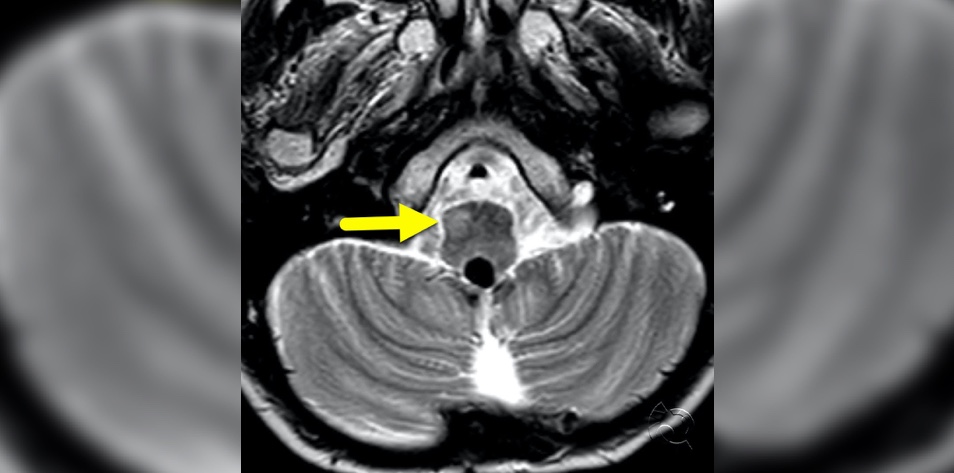
A 58-year-old comes to clinic six months after an ischemic stroke in the paramedian pontine reticular formation (PPRF). They initially present with acute vertigo, ataxia, and mild hemiplegia, which have significantly improved with therapy. The only complaint now is that a few weeks ago they developed an incessant clicking in the ears. The exam is noteworthy for continuous rapid spasms of the soft palate and increased nystagmus.
Repeat MRI demonstrates enlargement of the inferior olive with a new non-enhancing T2 hyperintensity. This is consistent with hypertrophic olivary degeneration, a form of multisynaptic transneuronal degeneration caused by disruption of the dento-rubro-olivary pathway (DROP) in the Guillain-Mollaret triangle. While strokes are a relatively common etiology of this rare condition, any lesion affecting these pathways can be implicated.
Cytoplasmic vacuolar degeneration and astrocytosis are seen in histopathology. The gross enlargement recedes into atrophy over years, although T2 hyperintensity is ongoing.
Palatal tremor and pendular nystagmus comprise the classic clinical features of a PPRF lesion. Dentorubral (Holm’s) tremor and ocular myoclonus may also be present. Mild symptoms are usually self-limited. For those with very bothersome palatal myoclonus, medical management is challenging. Clonazepam, anti-seizure medications, and botulinum toxin injection have been tried with some successes.
Further Reading
Figure 1 Medical Case: Hypertrophic Olivary Degeneration
MRI Findings in Nonlesional Hypertrophic Olivary Degeneration
References
Wang H, Wang Y, Wang R, Li Y, Wang P, Li J, Du J. Hypertrophic olivary degeneration: A comprehensive review focusing on etiology. Brain Res. 2019 Sep 1;1718:53-63. doi: 10.1016/j.brainres.2019.04.024. Epub 2019 Apr 23. PMID: 31026459.

Kaci McCleary, MD
Hospice and Palliative Care Fellow, OhioHealth
Published January 12, 2022
Want more clinical cases?
Join Figure 1 for free and start securely collaborating with other verified healthcare professionals on more than 100,000 real-world medical cases just like this one.