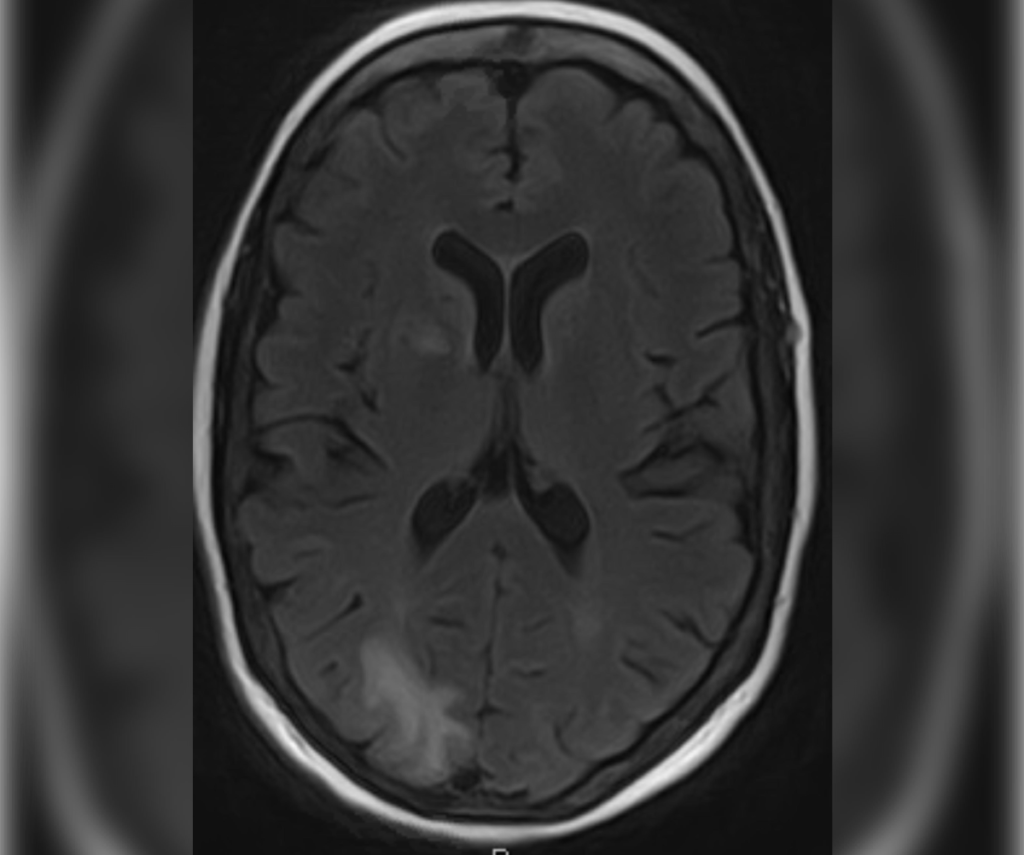
A 45-year-old with a history of HIV and variable adherence to antiretrovirals presents to the emergency department with slurred speech and vision changes and is found to have scattered white matter hyperintensities. While in the hospital, they continue to decline. The CD4 count on arrival was 130 cells/mm3 and viral load was 71,000 copies/mL.
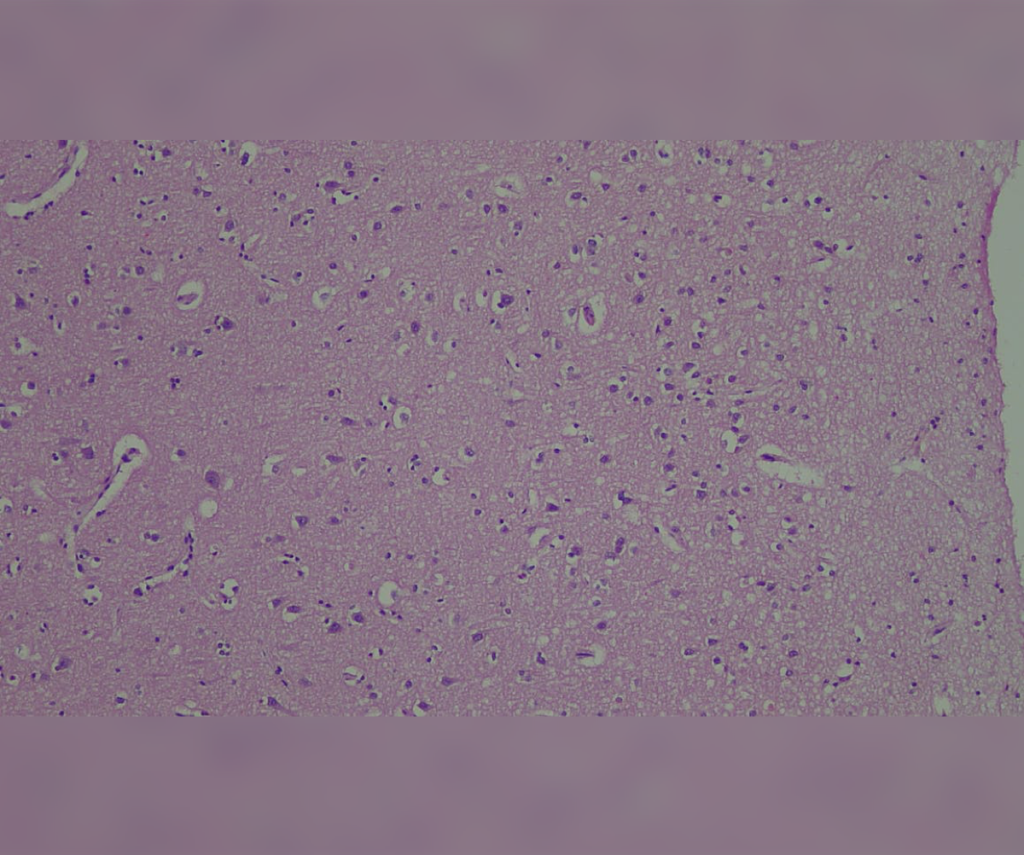
Brain biopsy shows H&E stain with bizarre astrocytes and enlarged oligodendroglial nuclei. SV40 immunostain cross-reacts to highlight JC viral inclusions. Other histological criteria include the presence of demyelination (Luxol blue stain) or visualization of viral particles using electron microscopy.
The patient is diagnosed with progressive multifocal leukoencephalopathy (PML). When histological evaluation is not possible, diagnosis can also be made based on typical clinical features, radiographic findings, and positive JC virus in CSF.
HIV/AIDS was historically the most common risk factor, although clinicians should maintain a high degree of suspicion when any immunosuppressed patient (leukemia/lymphoma, chemotherapy, post-transplant, immunotherapies like natalizumab), presents with unusual or progressive neurological findings.
Primary treatment is immune reconstitution by treating the underlying disease or changing/stopping offending medications. Morbidity and mortality are high.
Further Reading
References
Major, Eugene O. (2018). Progressive Multifocal Leukoencephalopathy Lesions and JC Virus: The Limits and Value of Imaging. JAMA Neurology, 75(7), 789-790.

Kaci McCleary, MD
Hospice and Palliative Care Fellow, OhioHealth
Published March 26, 2022
Want more clinical cases?
Join Figure 1 for free and start securely collaborating with other verified healthcare professionals on more than 100,000 real-world medical cases just like this one.