Learning Objective
- Understand the classic clinical findings, patterns of presentation and features of psoriatic arthritis.
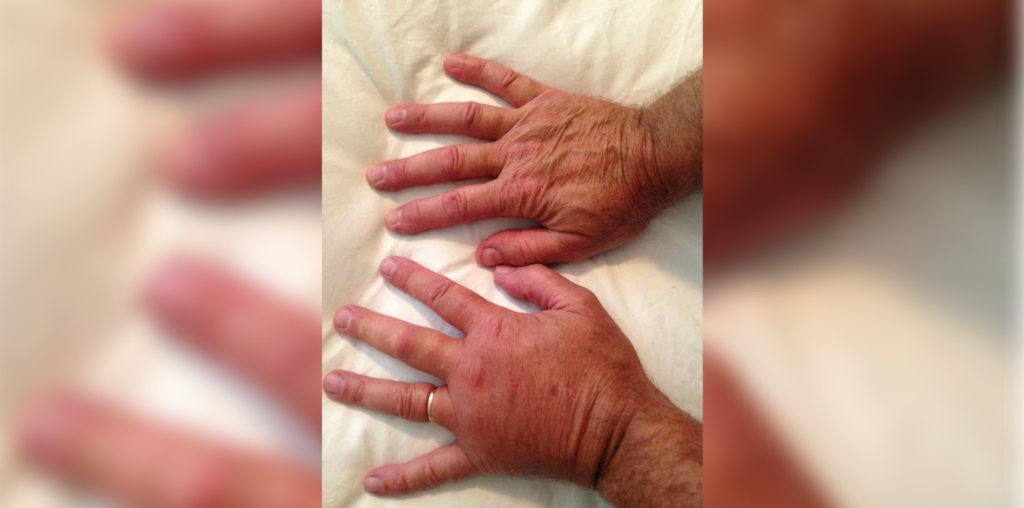
A 45-year-old presents with intermittent pain and joint swelling involving the left second, third, fourth and fifth distal interphalangeal joints, third proximal interphalangeal joint and left knee for the last two years. Symptoms usually improve with naproxen, but over the last six months, joint swelling and pain has become more persistent and the patient is concerned their fingers are getting more deformed. The patient reports morning stiffness of three hours. Patient also reports left low back and buttock pain, without radiation down the leg for which they take naproxen intermittently for the last three years.
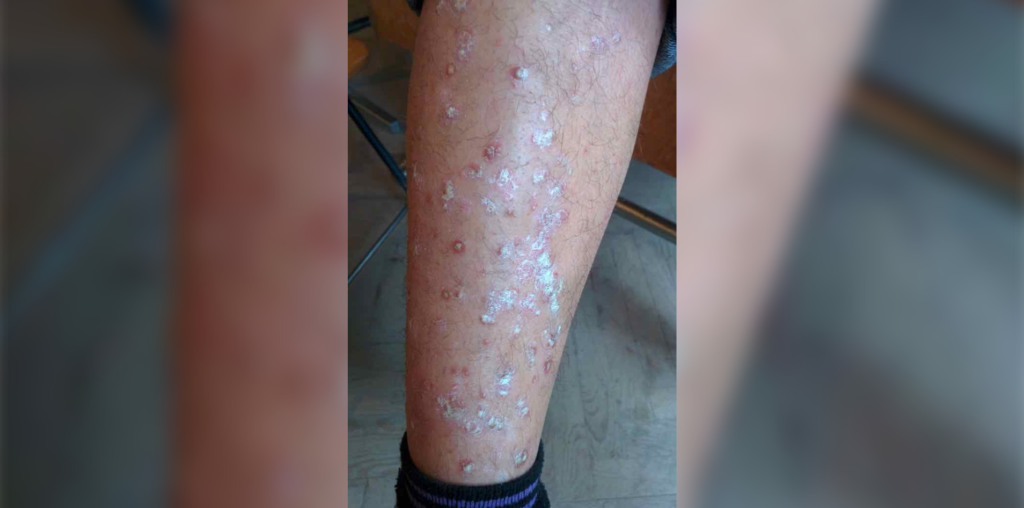
The patient reports a history of what they identify as eczema developing over the legs in the winter for the last two to three years, which improves in the summer. On exam, you note multiple scaly erythematous plaques over the anterior shins and also in the periumbilical area. You request hand, spine, and pelvic radiographs.
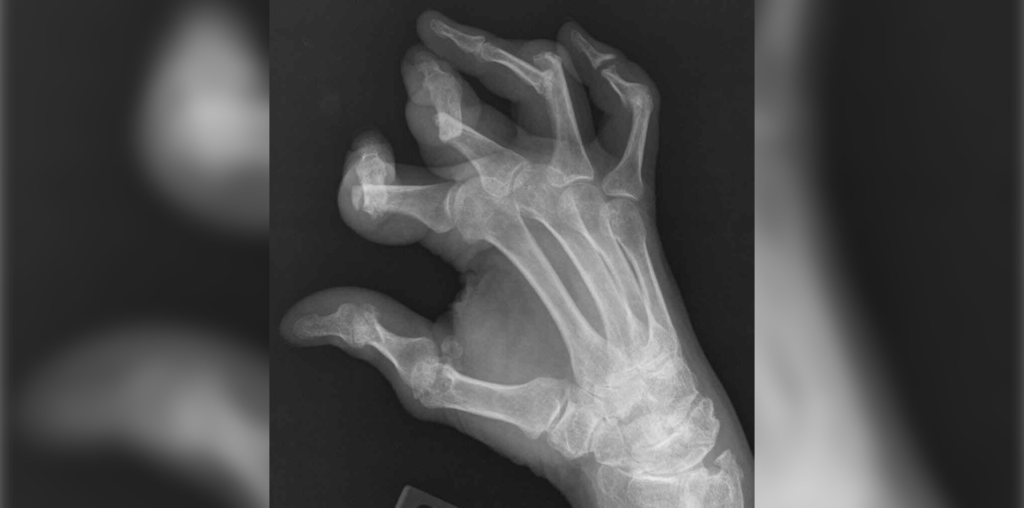
Periarticular erosions with new bone formation, bone resorption with ‘pencil-in-cup’ deformity and ankylosis are radiographic features suggestive of psoriatic arthritis, an inflammatory arthritis that affects 30% of patients with psoriasis. It typically develops following psoriasis, but in up to a third can precede the onset of skin disease. Peripheral arthritis can be oligoarticular, polyarticular, distal interphalangeal joint synovitis alone or arthritis mutilans. Inflammatory back pain from C- or L-spine spondylitis, or asymmetric sacroiliitis can also be seen. There are no diagnostic lab tests but rheumatoid factor and anti-CCP antibody are typically negative. Positive HLA-B27 can predispose to Psoriatic spondyoarthropathy and is associated with earlier age of psoriasis and arthritis onset, bilateral sacroiliitis, and those assigned male at birth.
Treatment options for psoriatic arthritis include NSAIDs, intermittent use of corticosteroids, disease modifying anti-rheumatic drugs, and biologics. Incorporating heat and cold therapy, splinting, and exercise can also relieve joint swelling and pain.
Further Reading
References
FitzGerald, O., Ogdie, A., Chandran, V. et al. Psoriatic arthritis. Nat Rev Dis Primers 7, 59 (2021). https://doi.org/10.1038/s41572-021-00293-y
Haddad A et al. Psoriatic Arthritis Mutilans: Clinical and Radiographic Criteria. A Systematic Review. The Journal of Rheumatology August 2015, 42 (8) 1432-1438; DOI: https://doi.org/10.3899/jrheum.141545
Queiro R, Sarasqueta C, Belzunegui J, Gonzalez C, Figueroa M, Torre-Alonso JC. Psoriatic spondyloarthropathy: a comparative study between HLA-B27 positive and HLA-B27 negative disease. Semin Arthritis Rheum. 2002 Jun;31(6):413-8. doi: 10.1053/sarh.2002.33470
Published September 28, 2022
Want more clinical cases?
Join Figure 1 for free and start securely collaborating with other verified healthcare professionals on more than 100,000 real-world medical cases just like this one.