A 15-year-old with a history of attention deficit hyperactivity disorder and autism presents to clinic for follow up after a first time generalized tonic-clonic seizure.
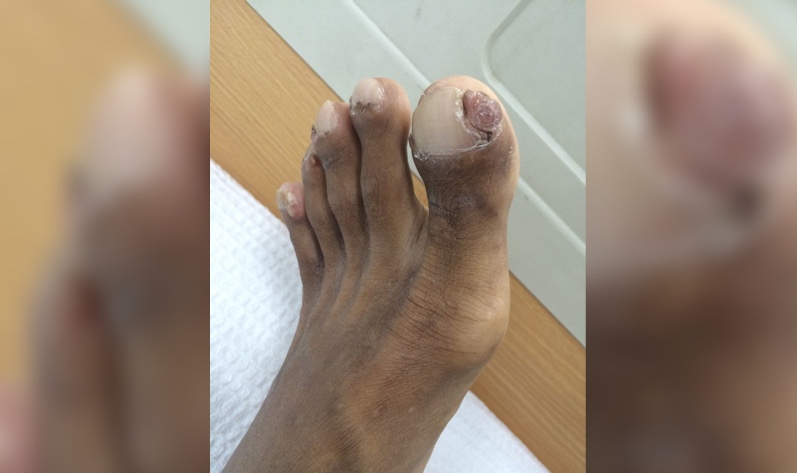
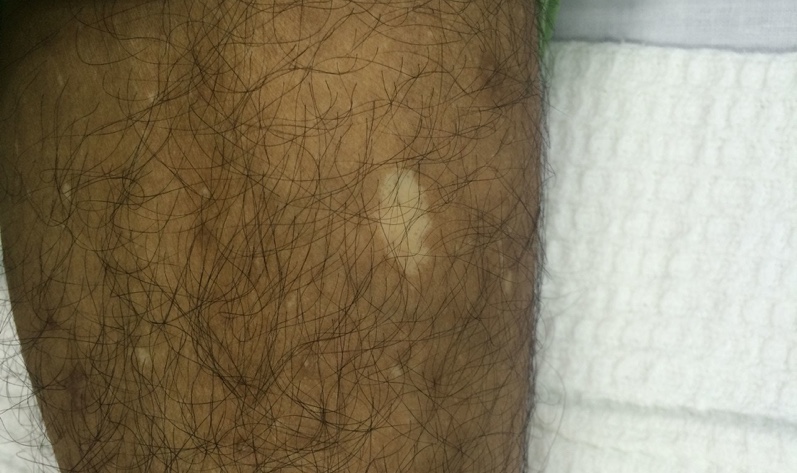
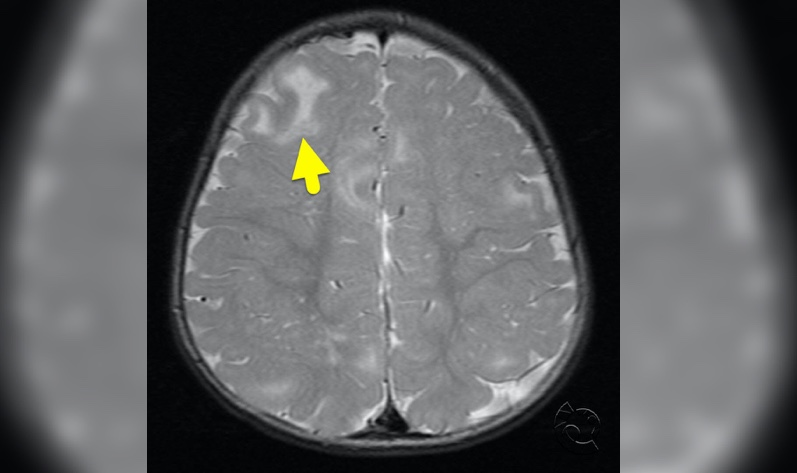
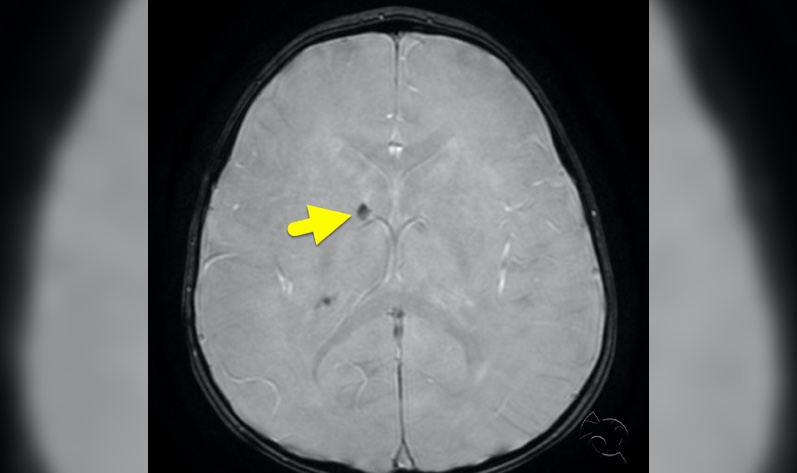
Physical exam is normal except hypomelanated “ash leaf spots” and periungual hamartomas (Koenen toes), as pictured. An MRI done as part of the seizure workup shows subcortical white matter changes (a “tuber”) on T2 and subependymal nodules on SWI, or susceptibility weighted imaging.
Tuberous sclerosis complex (TSC) is an autosomal dominant neurocutaneous disorder with complete penetrance but extremely variable clinical presentation. Over half of cases are caused by spontaneous mutations in individuals with negative family history.
Ash leaf spots are present at birth and are perhaps the most universal physical examination finding. Facial angiofibromas are also common. Seizures are the most common neurological complication and can be difficult to control in severe cases. Intellectual disability and behavioral issues are also frequently present, but up to half of patients will have normal cognitive development. All organ systems are at risk of hamartoma (“tuber”) development, so patients should be regularly screened for cardiovascular, pulmonary, renal, and ophthalmic involvement. Treatment primarily consists of resection of problematic tumors, although there is growing evidence for therapies affecting the mTOR pathway.
Diagnostic criteria require the presence of two major features or one major and two minor features. Genetic testing for TSC1/TSC2 is confirmatory.
Further Reading
Figure 1 medical case: Tuberous Sclerosis Complex
Figure 1 medical case: Tuberous Sclerosis Complex Imaging
Tuberous Sclerosis Complex: Recent Advances in Manifestations and Therapy
Tuberous Sclerosis Complex: Review Based on New Diagnostic Criteria
Reference
Leung AK, Robson WL. Tuberous sclerosis complex: a review. J Pediatr Health Care. 2007 Mar-Apr;21(2):108-14. doi: 10.1016/j.pedhc.2006.05.004. PMID: 17321910.

Kaci McCleary, MD
Hospice and Palliative Care Fellow, OhioHealth
Published December 10, 2021
Want more clinical cases?
Join Figure 1 for free and start securely collaborating with other verified healthcare professionals on more than 100,000 real-world medical cases just like this one.