Over the last several years there has been an increase in refusals to vaccinate, and this has been complicated with the spread of COVID-19. With this in mind, we asked over 1,000 healthcare professionals on Figure 1 how to talk to parents about vaccines when they have refused to vaccinate their children.
Of our respondents:
- 78% discuss the risk of severe illness
- 62% discuss the risk to vulnerable patients
- 53% refer to evidence-based studies
- 51% discuss the science of immunization
- 42% explain the concept of herd immunity
- 16% appeal to emotion with anecdotes
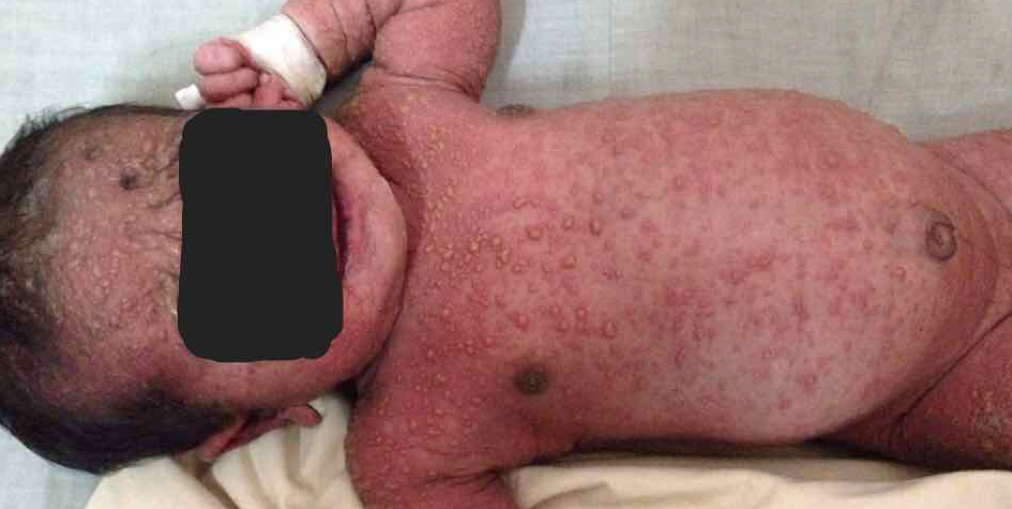
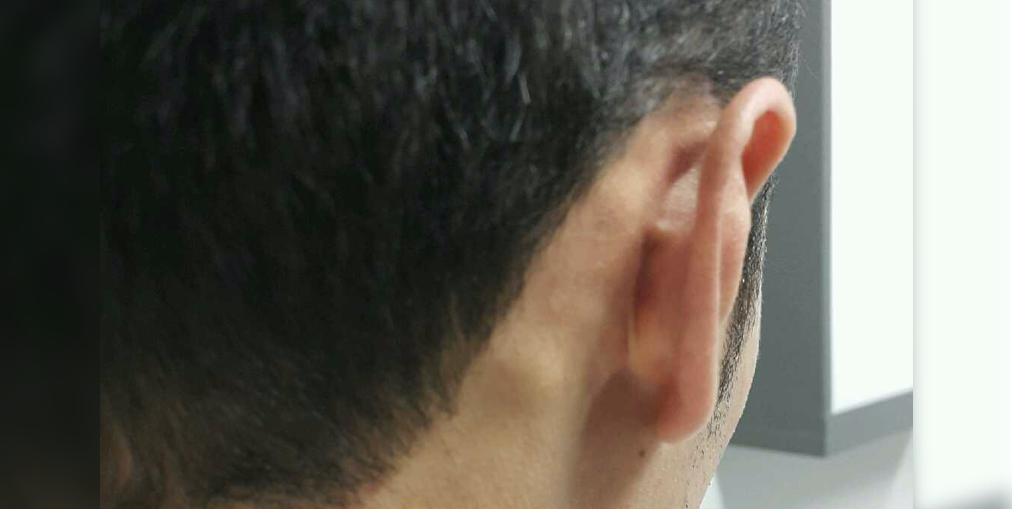
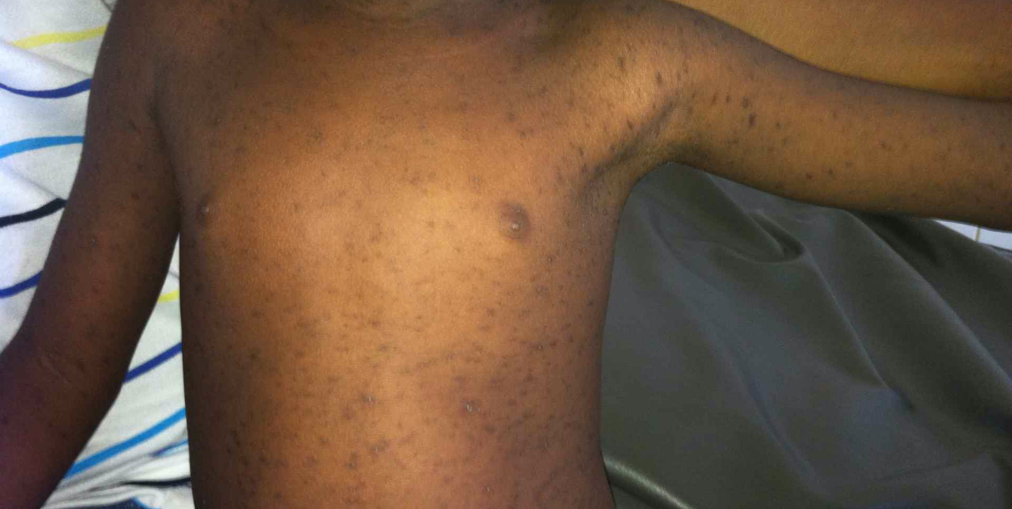
Chickenpox case, measles case, and rubella case
The community also provided the following five tips for how to talk to parents about vaccines.
1. Listen
The first rule of talking to a parent reluctant to vaccinate: stop talking. Understanding the parent’s concerns and ensuring they are heard is crucial.
“First of all, you have to listen to what they have to say, their fears, their beliefs, without judging: they love their child and just want the best for him/her.”
— Registered Nurse
“Show empathy, parents are fearful”
— General Practitioner
2. Know the Facts and the Fictions
“Stand firm. Repeat the scientific evidence. Educate yourself on the anti-vax arguments and have very specific responses to any of these mistruths that patients will throw at you …”
— General Practitioner
“Try to explain the science behind the benefits and the risks without aggressiveness. Also present the facts of the initial anti-vax reports and why they are not reliable sources.“
— Surgeon
3. Educate
Explain herd immunity, vulnerable populations, and relevant statistics. Show what polio, measles, and diphtheria can do to a child. Here are some real-life cases shared by the Figure 1 community. Cases like these can be used to educate parents on potential risks of avoiding vaccination.
4. Negotiate
Are there specific pain points you can minimize, perhaps with a modified schedule or different form of vaccine? Subtly underline the consequences of the decision.
“I give them the ‘walking through a firefight with no bulletproof vest’ analogy. I explain that it doesn’t mean the child will never get sick or have complications that are unforeseeable, it just means they have the best protection that can be given. It is not perfect, but none at all has been proven to be way more hazardous.”
— Registered Nurse
5. Keep Talking
For everyone’s health, an ongoing conversation is better than a closed door.
“Leave the door open for parents to change their minds. They may revisit the immunization question at next encounter”
— Neonatal Nurse
Published June 2021; updated November 29, 2021
Join the Conversation
Register for Figure 1 and be part of a global community of healthcare professionals gaining medical knowledge, securely sharing real patient cases, and improving outcomes.