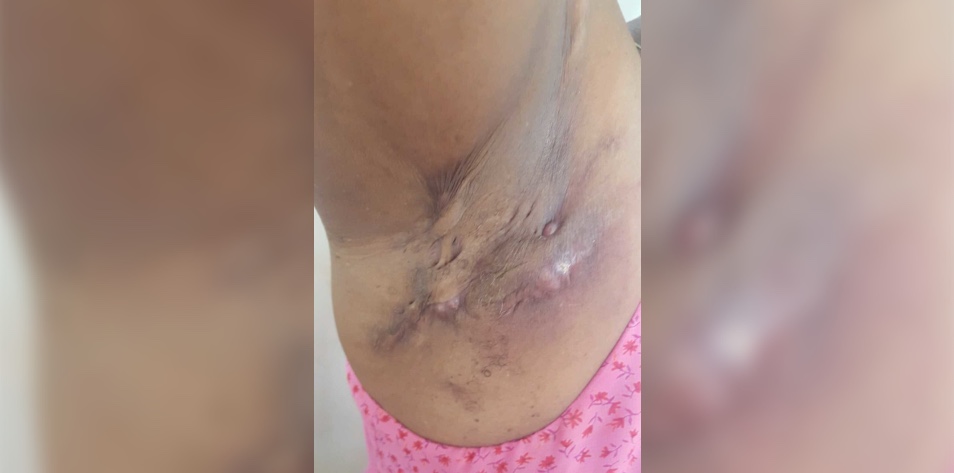
A 24-year-old with a history of bipolar disorder presents with an eruption of severe, progressive cystic lesions. Physical examination is remarkable for multiple actively draining nodules in the armpits, groin, and buttocks, which is clinically consistent with hidradenitis suppurativa, or HS.
About one month prior, the patient started lithium therapy for bipolar disorder, or BD. The serum lithium level measured within the therapeutic range. Given the acute concern for lithium-induced hidradenitis suppurativa, their psychiatrist discontinued the medication and changed to an alternative mood stabilizing agent. The patient was treated with a topical antiseptic wash, topical and oral antibiotics, and intralesional steroid injections. In follow up, they remain off the medication and demonstrate a gradual improvement in hidradenitis suppurative with a reduced number of lesions and frequency of flares.
HS is a chronic inflammatory skin condition characterized by inflammatory nodules, abscesses, comedones, sinus tracts, and scarring. The condition is significantly associated with increased prevalence of BD.
A population-based study by Tzur Bitan et al. and retrospective study by Benhadou et al. demonstrated an association between HS and BD. They reported increased prevalence of BD ranging from 0.6-0.7% in HS compared to 0.1% in matched controls. Tzur Bitan’s study demonstrated an increased proportion of active smoking in bipolar patients with HS compared to controls, which is a well-known risk factor for the skin condition. Benhadou’s study also demonstrated a temporal association between lithium therapy for bipolar disorder and the new-onset and/or worsening of hidradenitis suppurativa.
Although lesser known, there are several case reports of lithium-induced HS. The medication is commonly used for psychiatric conditions including BD, depression, and acute mania. It has a narrow therapeutic window and many associated systemic toxicities. Some of the most commonly reported adverse dermatologic side effects are psoriasis, acne, folliculitis, eczema, and hair loss. The pathophysiology is hypothesized to be similar to that of lithium-induced acne and psoriasis. The medication may promote neutrophilic inflammation and follicular occlusion by increasing circulating neutrophils, lysosomal enzyme release, and proliferation of keratinocytes. Related skin findings may be refractory to conventional therapies and require discontinuation of the medication.
While lithium-induced HS is lesser known, prompt recognition and multidisciplinary treatment may be needed to achieve adequate control of cutaneous and psychiatric symptoms in affected patients with complex comorbidities.
Further Reading
References
- Aithal V, Appaih P. Lithium induced hidradenitis suppurativa and acne conglobata. Indian J Dermatol Venereol Leprol. 2004 Sep-Oct;70(5):307-9. PMID: 17642646.
- Benhadou F, Villani AP, Guillem P. Hidradenitis Suppurativa and Bipolar Disorders: A Role for Lithium Therapy? Dermatology. 2020;236(4):305-306. doi: 10.1159/000505912. Epub 2020 Feb 7. PMID: 32036365.
- Gupta AK, Knowles SR, Gupta MA, Jaunkalns R, Shear NH. Lithium therapy associated with hidradenitis suppurativa: case report and a review of the dermatologic side effects of lithium. J Am Acad Dermatol. 1995 Feb;32(2 Pt 2):382-6. doi: 10.1016/0190-9622(95)90410-7. PMID: 7829746.
- Tzur Bitan D, Berzin D, Cohen A. Hidradenitis Suppurativa and Bipolar Disorders: A Population-Based Study. Dermatology. 2020;236(4):298-304. doi: 10.1159/000504535. Epub 2020 Jan 7. PMID: 31910425.
Want more clinical cases?
Join Figure 1 for free and start securely collaborating with other verified healthcare professionals on more than 100,000 real-world medical cases just like this one.